- Select a language for the TTS:
- UK English Female
- UK English Male
- US English Female
- US English Male
- Australian Female
- Australian Male
- Language selected: (auto detect) - EN
Play all audios:
ABSTRACT The 2004 UK Quality and Outcomes Framework (QOF) remunerates general practitioners for achieving a target blood pressure (BP) of ⩽150/90 mm Hg for patients with ischaemic heart
disease, stroke and hypertension. Using the DIN-LINK GP database, we investigated whether introducing the target altered BP recording. We extracted 3 164 189 BP measurements from 236 467
patients, with the above diagnoses from 2000 to 2005. Treatment was assessed by Read codes indicating prescriptions for antihypertensive drugs. Over this period, recorded systolic BP (SBP)
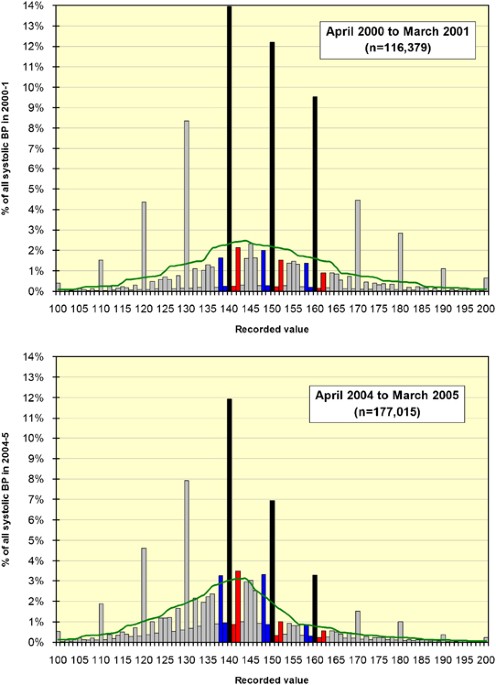
fell: 36% had an SBP >150 mm Hg in 2000–2001, and only 19% in 2004–2005. However, there was a trend towards recording systolic values just below, rather than just above the 150 cut-off.
In 2000–2001, 2.3% of patients had 148–149 recorded and 1.8% had 151–152. In 2004–2005, the figures were 4.2 and 1.3%, respectively. By smoothing the distribution we estimate that the true
percentage of patients with SBP>150 mm Hg in 2004–2005 was 23%, rather than the 19% recorded. Moreover, patients with a recorded SBP=148–149 were more likely to have a recorded diastolic
BP⩽90 (93%) than patients with SBP=151–152 (78%). However, patients just below the 150 mm Hg cut-off received more antihypertensive treatment than those just above it (odds ratio=1.20, 95%
confidence interval 1.01–1.41). We conclude that blood pressure levels in UK primary care have continued to fall through the introduction of QOF, offering significant public health benefits
in the future. This fall has been exaggerated due to values being clustered just below the QOF target, but there is no evidence of adverse effects of this on clinical management. Access
through your institution Buy or subscribe This is a preview of subscription content, access via your institution ACCESS OPTIONS Access through your institution Subscribe to this journal
Receive 12 digital issues and online access to articles $119.00 per year only $9.92 per issue Learn more Buy this article * Purchase on SpringerLink * Instant access to full article PDF Buy
now Prices may be subject to local taxes which are calculated during checkout ADDITIONAL ACCESS OPTIONS: * Log in * Learn about institutional subscriptions * Read our FAQs * Contact customer
support SIMILAR CONTENT BEING VIEWED BY OTHERS BLOOD PRESSURE MEASUREMENT TECHNIQUE IN CLINICAL PRACTICE IN THE NHS GREATER GLASGOW AND CLYDE Article Open access 05 December 2024 BLOOD
PRESSURE OUTCOMES AT 12 MONTHS IN PRIMARY CARE PATIENTS PRESCRIBED REMOTE PHYSIOLOGICAL MONITORING FOR HYPERTENSION: A PROSPECTIVE COHORT STUDY Article Open access 21 July 2023 VARIABILITY
IN HOME BLOOD PRESSURE AND ITS ASSOCIATION WITH RENAL FUNCTION AND PULSE PRESSURE IN PATIENTS WITH TREATED HYPERTENSION IN PRIMARY CARE Article Open access 15 November 2023 REFERENCES *
Department of Health, London UK. General Medical Services Contract. http://www.dh.gov.uk/en/Healthcare/Primarycare/Primarycarecontracting/GMS/DH_4125637, Last accessed: 11/7/08. * Shekelle P
. New contract for general practitioners. _BMJ_ 2003; 326: 457–458. Article PubMed PubMed Central Google Scholar * Graham I, Atar D, Borch-Johnsen K, Boysen G, Burell G, Cifkova R _et
al_. European guidelines on cardiovascular disease prevention in clinical practice: executive summary. _Eur Heart J_ 2007; 28: 2375–2414. Article PubMed Google Scholar * Wingfield D,
Cooke J, Thijs L, Staessen JA, Fletcher AE, Fagard R _et al_. Terminal digit preference and single-number preference in the Syst-Eur trial: influence of quality control. _Blood Press Monit_
2002; 7: 169–177. Article PubMed Google Scholar * Carey IM, DeWilde S, Harris T, Whincup PH, Cook DG . Spurious trends in coronary heart disease incidence: unintended consequences of the
new GP contract? _Br J Gen Pract_ 2007; 57: 486–489. PubMed PubMed Central Google Scholar * Heath I, Hippisley-Cox J, Smeeth L . Measuring performance and missing the point? _BMJ_ 2007;
335: 1075–1076. Article PubMed PubMed Central Google Scholar * Primatesta P, Brookes M, Poulter NR . Improved hypertension management and control: results from the health survey for
England 1998. _Hypertension_ 2001; 38: 827–832. Article CAS PubMed Google Scholar * Carey IM, Cook DG, De Wilde S, Bremner SA, Richards N, Caine S _et al_. Developing a large electronic
primary care database (Doctors’ Independent Network) for research. _Int J Med Inform_ 2004; 73: 443–453. Article PubMed Google Scholar * Lusignan S, Sismanidis C, Carey IM, DeWilde S,
Richards N, Cook DG . Trends in the prevalence and management of diagnosed type 2 diabetes 1994–2001 in England and Wales. _BMC Fam Pract_ 2005; 6: 13. Article PubMed PubMed Central
Google Scholar * DeWilde S, Carey IM, Emmas C, Richards N, Cook DG . Trends in the prevalence of diagnosed atrial fibrillation, its treatment with anticoagulation and predictors of such
treatment in UK primary care. _Heart_ 2006; 92: 1064–1070. Article CAS PubMed Google Scholar * De Wilde S, Carey IM, Bremner SA, Richards N, Hilton SR, Strachan DP _et al_. A comparison
of the recording of 30 common childhood conditions in the Doctor's Independent Network and General Practice Research Databases. _Health Stat Q_ 2004; 22: 21–31. Google Scholar * Health
Survey for England. Trends in blood pressure levels. http://www.heartstats.org/datapage.asp?id=1000, Last accessed: 11/7/08. * DeWilde S, Carey IM, Richards N, Whincup PH, Cook DG . Trends
in secondary prevention of ischaemic heart disease in the UK 1994–2005: use of individual and combination treatment. _Heart_ 2008; 94: 83–88. Article CAS PubMed Google Scholar * Ashworth
M, Medina J, Morgan M . Effect of social deprivation on blood pressure monitoring and control in England: a survey of data from the quality and outcomes framework. _BMJ_ 2008; 337: a2030.
Article PubMed PubMed Central Google Scholar * De Lusignan S, Belsey J, Hague N, Dzregah B . End-digit preference in blood pressure recordings of patients with ischaemic heart disease in
primary care. _J Hum Hypertens_ 2004; 18: 261–265. Article CAS PubMed Google Scholar * Beales D . How accurate are automated blood pressure monitors? _Br J Community Nurs_ 2005; 10:
334–338. Article PubMed Google Scholar * McManus RJ, Mant J, Hull MR, Hobbs FD . Does changing from mercury to electronic blood pressure measurement influence recorded blood pressure? An
observational study. _Br J Gen Pract_ 2003; 53: 953–956. PubMed PubMed Central Google Scholar * Harrison WN, Lancashire RJ, Marshall TP . Variation in recorded blood pressure terminal
digit bias in general practice. _J Hum Hypertens_ 2008; 22 (3): 163–167. Article CAS PubMed Google Scholar * Manning G, Brooks A, Slinn B, Millar-Craig MW, Donnelly R . Assessing blood
pressure control in patients treated for hypertension: comparing different measurements and targets. _Br J Gen Pract_ 2006; 56: 375–377. PubMed PubMed Central Google Scholar * Wingfield
D, Freeman GK, Bulpitt CJ . Selective recording in blood pressure readings may increase subsequent mortality. _QJM_ 2002; 95: 571–577. Article CAS PubMed Google Scholar * Nietert PJ,
Wessell AM, Feifer C, Ornstein SM . Effect of terminal digit preference on blood pressure measurement and treatment in primary care. _Am J Hypertens_ 2006; 19: 147–152. Article PubMed
Google Scholar Download references ACKNOWLEDGEMENTS We acknowledge with gratitude the general practitioners who provided the data to the DIN-LINK. We are grateful to Cegedim Strategic Data
(Woking, Surrey, UK) for their technical assistance with DIN-LINK database and for their helpful support. IMC and SDW were funded by a grant from the BUPA Foundation. AUTHOR INFORMATION
AUTHORS AND AFFILIATIONS * Division of Community Health Sciences, St George's, University of London, London, UK I M Carey, C M Nightingale, S DeWilde, T Harris, P H Whincup & D G
Cook Authors * I M Carey View author publications You can also search for this author inPubMed Google Scholar * C M Nightingale View author publications You can also search for this author
inPubMed Google Scholar * S DeWilde View author publications You can also search for this author inPubMed Google Scholar * T Harris View author publications You can also search for this
author inPubMed Google Scholar * P H Whincup View author publications You can also search for this author inPubMed Google Scholar * D G Cook View author publications You can also search for
this author inPubMed Google Scholar CORRESPONDING AUTHOR Correspondence to I M Carey. RIGHTS AND PERMISSIONS Reprints and permissions ABOUT THIS ARTICLE CITE THIS ARTICLE Carey, I.,
Nightingale, C., DeWilde, S. _et al._ Blood pressure recording bias during a period when the Quality and Outcomes Framework was introduced. _J Hum Hypertens_ 23, 764–770 (2009).
https://doi.org/10.1038/jhh.2009.18 Download citation * Received: 14 November 2008 * Revised: 28 January 2009 * Accepted: 30 January 2009 * Published: 12 March 2009 * Issue Date: November
2009 * DOI: https://doi.org/10.1038/jhh.2009.18 SHARE THIS ARTICLE Anyone you share the following link with will be able to read this content: Get shareable link Sorry, a shareable link is
not currently available for this article. Copy to clipboard Provided by the Springer Nature SharedIt content-sharing initiative KEYWORDS * blood pressure * measurement bias * quality and
outcomes * general practice








